A HOSPITAL has denied putting a patient in a store room, after she complained of "diabolical" treatment.
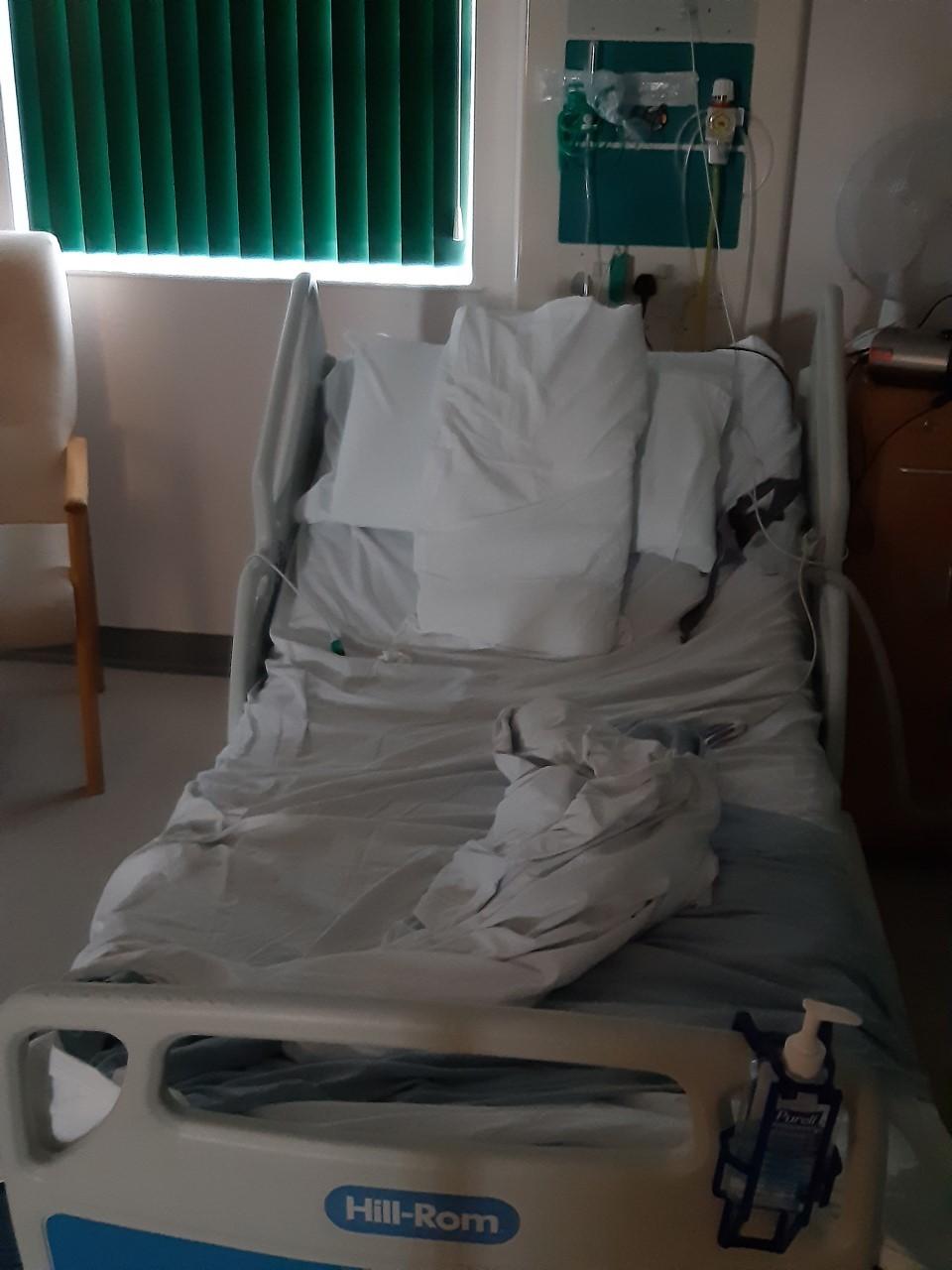
Jill Cooper said she was put in the room containing boxes for 22 hours when she went into Worcestershire Royal Hospital with suspected appendicitis.
Mrs Cooper, 57, said she waited over seven hours to see a doctor.
She rang the Worcester News from the hospital.
She said: “I am in a lot of pain. It’s diabolical, I wouldn’t treat my puppy like this. It’s just awful.
“I ring the bell for a nurse and I have told the staff that my medication isn’t helping the pain. It’s absolutely mad.”
Mrs Cooper, a bookkeeper from Droitwich, added: “I have worked all my life – if this is the NHS, it is diabolical.
“People were coming in and out taking things from cupboards.”
Mrs Cooper, who was discharged after blood tests, said she was moved on to a ward after two nights in the room.
The trust said it was sorry Mrs Cooper was dissatisfied with her care.
A spokesman for Worcestershire Acute Hospitals NHS Trust said: “We would never use a store room for patient care. Our doctors, nurses and other staff are working hard to care for high numbers of people in need or urgent and emergency care.
“We have taken steps to make sure we see patients as quickly as we can, prioritising those who are most unwell. Patients may sometimes be temporarily placed in treatment rooms used for surgical decisions rather than traditional ward bays or side rooms. We don’t treat patients in store rooms and a patient’s clinical care will not be compromised by the room they are placed in.
"However, our focus is always on putting patients first and we are sorry if Mrs Cooper’s experience of care was not up to the high standards that we set for ourselves. We recently launched a new surgical assessment pathway meaning that patients with surgical needs can be moved out of A&E to a dedicated assessment area where they can be assessed more quickly rather than waiting longer to be seen in A&E.
“An additional £730,000 has also been secured by commissioners to increase capacity in the community to enable an additional 40 patients a week to be safely discharged back to their own home with care support.”




Comments: Our rules
We want our comments to be a lively and valuable part of our community - a place where readers can debate and engage with the most important local issues. The ability to comment on our stories is a privilege, not a right, however, and that privilege may be withdrawn if it is abused or misused.
Please report any comments that break our rules.
Read the rules hereLast Updated:
Report this comment Cancel